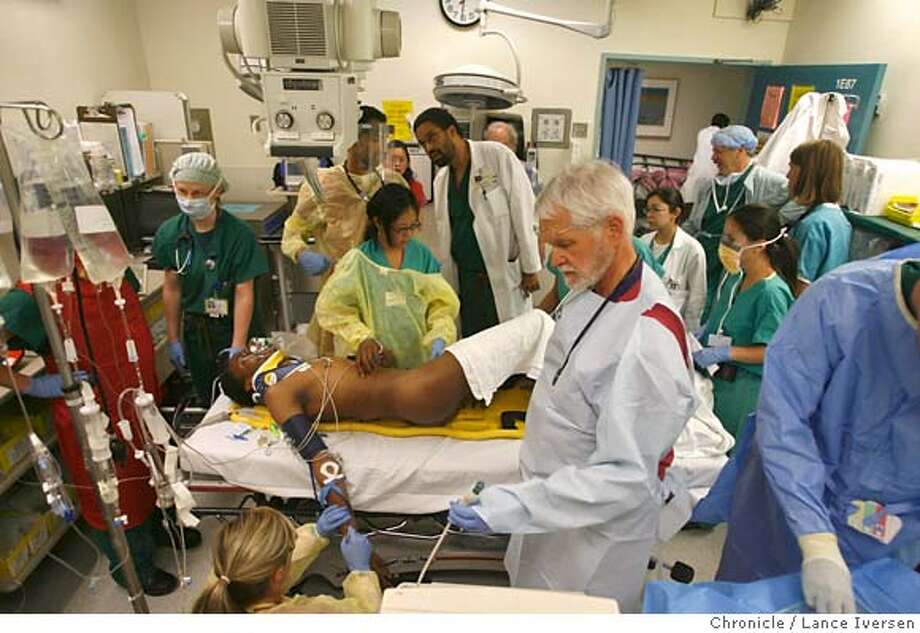
Keep unconscious children in the recovery position. Keep the child under observation for 4–24 h, depending on the poison swallowed. Give a specific antidote if this is indicated. Note that tracheal intubation by an anaesthetist may be required to reduce the risk of aspiration. Lavage should be continued until the recovered lavage solution is clear of particulate matter. The volume of lavage fluid returned should approximate the amount of fluid given. Perform lavage with 10 ml/kg of normal saline (0.9%). Pass a 24–28 French gauge tube through the mouth into the stomach, as a smaller nasogastric tube is not sufficient to let particles such as tablets pass. 
Measure the length of tube to be inserted. Place the child in the left lateral head-down position. Make sure a suction apparatus is available in case the child vomits. Undertake gastric lavage only if staff have experience in the procedure, if ingestion was less than 1 h previously and is life-threatening and if the child did not ingest corrosives or petroleum derivatives. Treatment is most effective if given as quickly as possible after the poisoning event, ideally within 1 h. Identify the specific agent and remove or adsorb it as soon as possible. Ingestion of corrosives or petroleum products ►Ĭheck the child for emergency signs and for hypoglycaemia if blood glucose is not available and the child has a reduced level of consciousness, treat as if hypoglycaemia. Gastric decontamination does not guarantee that all the substance has been removed, so the child may still be in danger.Ĭontraindications to gastric decontamination are: –Īn unprotected airway in an unconscious child, except when the airway has been protected by intubation with an inflated tube by the anaesthetist – A decision to undertake gastric decontamination must weigh the likely benefits against the risks associated with each method. After this time, there is usually little benefit, except for agents that delay gastric emptying or in patients who are deeply unconscious. Gastric decontamination is most effective within 1 h of ingestion. Ingested poisons must be removed from the stomach. Corrosives can cause oesophageal burns, which may not be immediately apparent, and petroleum products, if aspirated, can cause pulmonary oedema, which may take some hours to develop.Īll children who present as poisoning cases should quickly be assessed for emergency signs (airway, breathing, circulation and level of consciousness), as some poisons depress breathing, cause shock or induce coma. ►Ĭhildren who have ingested corrosives or petroleum products should not be sent home without observation for at least 6 h. ►Īdmit all children who have deliberately ingested iron, pesticides, paracetamol or aspirin, narcotics or antidepressant drugs and those who may have been given the drug or poison intentionally by another child or adult. ■Ĭheck for signs of burns in or around the mouth or of stridor (upper airway or laryngeal damage), which suggest ingestion of corrosives. 
The symptoms and signs depend on the agent ingested and therefore vary widely – see below. Check that no other children were involved. Attempt to identify the exact agent involved and ask to see the container, when relevant. Obtain full details of the poisoning agent, the amount ingested and the time of ingestion. Shock (can cause lethargy or unconsciousness, but is unlikely to cause convulsions)Īcute glomerulonephritis with encephalopathyĪ diagnosis is based on a history from the child or carer, a clinical examination and the results of investigations, where appropriate. History of poison ingestion or drug overdose severe malaria and treat the cause to prevent a recurrence)īlood glucose low (< 2.5 mmol/litre (< 45 mg/dl) or < 3.0 mmol/litre (< 54 mg/dl) in a severely malnourished child) responds to glucose treatment Hypoglycaemia (always seek the cause, e.g. Prior episodes of short convulsions when febrile – falciparum often seasonal)īlood smear or rapid diagnostic test positive for malaria parasites –įebrile convulsions (not likely to be the cause of unconsciousness) Petaechial rash (meningococcal meningitis only) –Ĭerebral malaria (only in children exposed to P.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
